Contact Us
Medical Laboratory Science
127 Halsey Science Center
(920) 424-1487
More contact information
Elementary Hematology
BLOOD. It is one of the biggest fear factors in every horror movie, and the very sight of it can make some people faint!
Blood is vital to life. It can travel through your circulatory system up to 10 miles every hour, bathing every cell in the body in 20 seconds.
Because it is such a powerful and important fluid, blood has been carefully studied for centuries.
Frequently Asked Questions
What Is Hematology?
“Hematology” comes from the Greek words haima, meaning blood, and logos, meaning study or science. So, hematology is the science of blood.
Blood is very different from other body tissue. Your blood is made of a solid and a liquid portion. The liquid portion is called plasma. The solid portion is comprised of cells.
Cells are the basic units of life. All living organisms are made of one or many cells. Unicellular organisms like bacteria are made of just one cell. Multicellular organisms, like plants and animals, are made of more than one cell. The human body has over 75 trillion cells!
Cells are so small they must be studied under a microscope to be seen. Bacteria are prokaryotic cells that have no nucleus. Most other living things are made of eukaryotic cells, which have a nucleus and organelles. Organelles are organized structures found in or on cells. The nucleus, the largest organelle, contains chromosomes and stores all the genetic information for the cell. Other organelles make proteins, produce energy, or store wastes. Most organelles are surrounded by membranes that let some substances into the cell while keeping others out. Each cell has a cytoskeleton that gives it shape and may help it move. The cell’s cytoplasm (cytosol) surrounds the nucleus and organelles. The entire cell is surrounded by a plasma membrane, which works like the organelle membranes, letting some substances in and keeping others out. The ability to select what comes into the cell is known as being semi-permeable.
Most cells share these basic common characteristics, but in multicellular organisms (like people) each cell also performs a specialized function. Your blood cells are very specialized. Blood is the only tissue made of cells that do not stick together. Other tissues like muscle, skeleton, and nerves are made of cells that join together to work together as a tissue. Blood cells, on the other hand, are designed to float separately throughout your body inside vessels called arteries and veins. Some blood cells can carry oxygen from your lungs to your tissues. Some are able to fight infection, while others can repair the arteries and veins they travel through. There are three main categories of blood cells: white blood cells, red blood cells, and platelets. Each has a particular job in your blood.
When your blood cells aren’t doing their jobs correctly, it can make you sick. There are many different problems that can occur to make your blood cells perform poorly. A person who studies hematology can recognize what type of problem there is with the sick blood cells and why it is happening.
Who Studies Hematology?
Many people use hematology in their careers.
Research scientists use their curiosity and creativity to discover the answers to questions we still have about our blood and circulatory system. For example, can we predict when a person may have a heart attack?
Teachers study hematology, take their knowledge of blood and pass it on to their students.
Artists who draw for medical texts must understand the structure of blood cells in order to depict them accurately.
Doctors use their knowledge of hematology to diagnose and treat disease. The doctor gets help from medical laboratory scientists who specialize in the study of blood.
Medical laboratory scientists actually work with human blood, studying it first hand. They evaluate it under microscopes and with automated instruments. These instruments can count cells and measure how long it takes for blood to clot. The medical laboratory scientist is asked to produce data and information that will aid in diagnosis, management, and treatment of disease.
The engineers who design hematology instruments must also have an understanding of hematology so that they can make their equipment the best possible for medical laboratory scientists to use.
The Five Common White Blood Cells
White blood cells – or leukocytes (lu’-ko-sites) – protect the body against infectious disease. These cells are colorless, but we can use special stains on the blood that make them colored and visible under the microscope.
White blood cells are the largest blood cell and can move by sticking out one part of their body and dragging the rest of themself along. They are the “soldiers” of the blood, attacking bacteria and other invaders unfamiliar to the body. White blood cells are able to squeeze through tiny blood vessels, leaving the bloodstream to enter other tissues that are being attacked by foreign invaders.
Most white blood cells are manufactured in the red marrow of bones. Some are also made in special glands elsewhere in the body. In a healthy person, there are between 4 and 11 thousand leukocytes in every cubic inch of blood. When a person has an infection, this signals the marrow and special glands to make more white blood cells. When a medical laboratory scientist counts the white blood cells in someone’s blood, they can tell the doctor if there is an infection.
There are five types of white blood cells. They are neutrophils, eosinophils, basophils, lymphocytes, and monocytes. These five types are in two main groups: The Granulocytes and The Mononuclear Cells.
Neutrophils
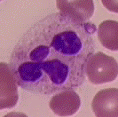 The neutrophils make up the majority of the total white blood cells in a normal person’s blood. Of the total white blood cells, there are usually 50-70 percent neutrophils. A mature neutrophil has a segmented nucleus and is twice the size of a red blood cell. A segmented nucleus means that you can see two to five segments (aka- lobes) of nucleus in one cell.
The neutrophils make up the majority of the total white blood cells in a normal person’s blood. Of the total white blood cells, there are usually 50-70 percent neutrophils. A mature neutrophil has a segmented nucleus and is twice the size of a red blood cell. A segmented nucleus means that you can see two to five segments (aka- lobes) of nucleus in one cell.
Neutrophils, eosinophils, and basophils are all granulocytes because they contain granules. The granules in a 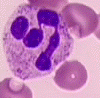 neutrophil are small, numerous, and are stained a light-pink to bluish-purple, “neutral” color. The cytoplasm of a neutrophil is light pink. When a person is fighting infection, the granules may be dark colored. This is called toxic granulation. One type of anemia causes the neutrophils to be hyperlobulated. This means that many of the neutrophils have six or more lobes to their nucleus. Whenever a person experiences any kind of inflammation, the neutrophils are the first to the scene.
neutrophil are small, numerous, and are stained a light-pink to bluish-purple, “neutral” color. The cytoplasm of a neutrophil is light pink. When a person is fighting infection, the granules may be dark colored. This is called toxic granulation. One type of anemia causes the neutrophils to be hyperlobulated. This means that many of the neutrophils have six or more lobes to their nucleus. Whenever a person experiences any kind of inflammation, the neutrophils are the first to the scene.
Eosinophils
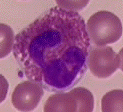 Eosinophils are also granulocytes…so they have granules, too! Their granules are different from neutrophil granules, though. The suffix “phil” means “to love”. Eosin is a type of acid red dye. Therefore, eosinophils love eosin dye. They grab onto lots of eosin dye when they’re stained, making their large granules a red color. The granules in an eosinophil usually cover the nucleus, but sometimes you can see that the nucleus is segmented. Eosinophils are not as common in the blood as neutrophils. They’re usually less than three percent of a person’s total white blood cells. Unless you have allergies…..then they come out to fight! Depending on the severity of the allergic reaction, they can be in much higher percentages. Although their primary job is to be involved in allergic reactions, eosinophils are also increased when a person has a parasite. For example, a person with a tapeworm in their digestive tract will have an elevated eosinophil count.
Eosinophils are also granulocytes…so they have granules, too! Their granules are different from neutrophil granules, though. The suffix “phil” means “to love”. Eosin is a type of acid red dye. Therefore, eosinophils love eosin dye. They grab onto lots of eosin dye when they’re stained, making their large granules a red color. The granules in an eosinophil usually cover the nucleus, but sometimes you can see that the nucleus is segmented. Eosinophils are not as common in the blood as neutrophils. They’re usually less than three percent of a person’s total white blood cells. Unless you have allergies…..then they come out to fight! Depending on the severity of the allergic reaction, they can be in much higher percentages. Although their primary job is to be involved in allergic reactions, eosinophils are also increased when a person has a parasite. For example, a person with a tapeworm in their digestive tract will have an elevated eosinophil count.
Basophils
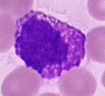
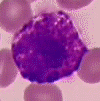 Basophils, the last and least (in number) of the granulocytes. They are present as one percent or less of a person’s white blood cells. Just like the eosinophils, basophils love dye. But, basophils love “basic blue” dye. Therefore, their large granules are a deep blue-purple color. Their nucleus is also segmented, but it’s hard to see in the presence of those intense granules!
Basophils, the last and least (in number) of the granulocytes. They are present as one percent or less of a person’s white blood cells. Just like the eosinophils, basophils love dye. But, basophils love “basic blue” dye. Therefore, their large granules are a deep blue-purple color. Their nucleus is also segmented, but it’s hard to see in the presence of those intense granules!
Lymphocytes
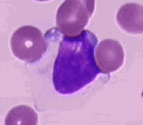 The lymphocytes and monocytes belong to the mononuclear cell group. This means their nucleus is in one piece. Lymphocytes are the main cells in the lymph nodes. There are almost as many lymphocytes as neutrophils in the blood. Lymphocytes are special because they can become “memory cells”. When doctors talk about a person being “immune”, they are referring to the ability of that person’s lymphocytes to remember a foreign invader. When a person is exposed to a new infectious agent, some of their lymphocytes make antibodies against it. The rest of the lymphocytes remember that infectious agent and get the immune system working faster the next time a person is exposed to that infectious agent. Very young children have more lymphocytes than adults because they are developing immunity to the many new infectious agents around them. Lymphocytes make up 20-40 percent of an adult’s total white blood cells.
The lymphocytes and monocytes belong to the mononuclear cell group. This means their nucleus is in one piece. Lymphocytes are the main cells in the lymph nodes. There are almost as many lymphocytes as neutrophils in the blood. Lymphocytes are special because they can become “memory cells”. When doctors talk about a person being “immune”, they are referring to the ability of that person’s lymphocytes to remember a foreign invader. When a person is exposed to a new infectious agent, some of their lymphocytes make antibodies against it. The rest of the lymphocytes remember that infectious agent and get the immune system working faster the next time a person is exposed to that infectious agent. Very young children have more lymphocytes than adults because they are developing immunity to the many new infectious agents around them. Lymphocytes make up 20-40 percent of an adult’s total white blood cells.
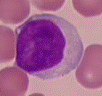 Small lymphocytes have a round nucleus and a small amount of blue cytoplasm. Overall, the lymphocyte looks very smooth and round. Lymphocytes vary a lot. They can be larger with a lot of cytoplasm when they are encountering an infectious agent. Sometimes they can even look wavy, like a potato chip!
Small lymphocytes have a round nucleus and a small amount of blue cytoplasm. Overall, the lymphocyte looks very smooth and round. Lymphocytes vary a lot. They can be larger with a lot of cytoplasm when they are encountering an infectious agent. Sometimes they can even look wavy, like a potato chip!
Monocytes
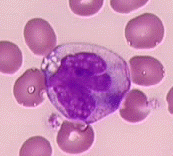 Monocytes serve as part of the defense against infection by “eating” up foreign particles. When a monocyte is found in tissue, it is called a macrophage.
Monocytes serve as part of the defense against infection by “eating” up foreign particles. When a monocyte is found in tissue, it is called a macrophage.
Monocytes are large cells- three to four times the size of a red blood cell! However, there are not too many in the bloodstream. In a normal person, there are one to six percent monocytes. Monocytes can be difficult to differentiate from lymphocytes. Monocytes usually have a larger amount of cytoplasm in relation to the size of the nucleus. They are also usually more irregular in shape than the smooth lymphocytes. You can sometimes see “pseudopods” on monocytes, the “fake feet” that help it move 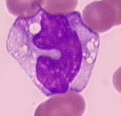 and digest foreign particles. The cytoplasm of a monocyte is a dull blue-gray color. Even though they are not granulocytes, monocytes have granules! They are very fine and lightly stained, giving the monocyte cytoplasm a “ground-glass” appearance. You may also see vacuoles. These look like holes in the cytoplasm. When a monocyte has vacuoles, you know it has been hard at work. The vacuoles contain chemicals that digest the foreign particles. The nucleus of the monocyte is usually kidney-shaped and has brain-like convolutions (ie- the nucleus looks like it’s folded).
and digest foreign particles. The cytoplasm of a monocyte is a dull blue-gray color. Even though they are not granulocytes, monocytes have granules! They are very fine and lightly stained, giving the monocyte cytoplasm a “ground-glass” appearance. You may also see vacuoles. These look like holes in the cytoplasm. When a monocyte has vacuoles, you know it has been hard at work. The vacuoles contain chemicals that digest the foreign particles. The nucleus of the monocyte is usually kidney-shaped and has brain-like convolutions (ie- the nucleus looks like it’s folded).
Red Blood Cells and Platelets
Red blood cell – or erythrocytes (e-rith’ro-sites) – make up about 45 percent of the solid part of the blood. In a healthy person, there are approximately 5.5 million red blood cells per cubic inch of blood. This means red blood cells out number white blood cells 1,000 to 1. Erythrocytes are disc-shaped cells that have no nucleus. They are made mostly of hemoglobin, a protein that contains iron and a pigment that causes blood to have its red color.
The function of erythrocytes is to pick up oxygen at the lungs and carry it to the tissues. Red blood cells are the “distributors” of the blood, carrying oxygen to the tissues and taking carbon dioxide (a waste product) from the tissues to the lungs where it is exhaled. The hemoglobin is the part of the erythrocyte that actually carries the oxygen and carbon dioxide.
Red blood cells are made in the red marrow of bones, and live about 120 days. Because they wear out so quickly, an entire supply of red blood cells is renewed every four months. As red blood cells wear out in the bloodstream, they are taken in by the spleen, an organ on the left side of the abdomen below the stomach, and destroyed. Parts of the old cells are salvaged to make new red blood cells.
The picture below shows what a blood smear looks like under a microscope. The many red disks are red blood cells. The purple cell in the center is a white blood cell.
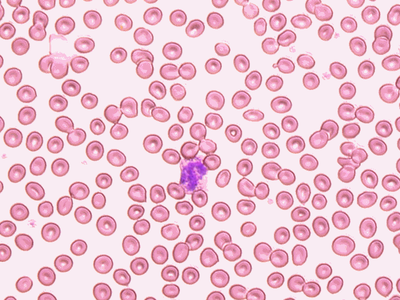 Medical laboratory scientists are often asked to count the number of red blood cells in a patient’s blood and evaluate their shape and color. Instruments are available that will automatically count the number of cells. The technologist looks at a blood smear under a microscope to evaluate the shape and color of the cells.
Medical laboratory scientists are often asked to count the number of red blood cells in a patient’s blood and evaluate their shape and color. Instruments are available that will automatically count the number of cells. The technologist looks at a blood smear under a microscope to evaluate the shape and color of the cells.
A common disorder of red blood cells is anemia. Anemia is a broad term used to describe all diseases where a person has decreased amounts of hemoglobin, and usually not enough red blood cells. The color and shape of the person’s red blood cells can tell a technologist or doctor what type of anemia the person has.
There are many different types of anemia. Some anemia may not cause problems unless people exert themselves. These people may have trouble breathing during exercise, and usually appear pale. Other, more severe, anemia can cause muscle cramping, dizziness, fatigue, and insomnia. The most severe anemia may cause coma and death. Such severe symptoms occur because oxygen is not getting to tissues and waste products are building up in the tissues. Think of it as a restaurant that didn’t hire enough wait staff: a few waiters (i.e.- red blood cells) are running around like crazy trying to get the food (i.e.- oxygen) out to the customers (i.e.- tissue cells) and clear tables (i.e.- remove wastes). The dirty dishes pile up on tables and food sits back in the kitchen (i.e.- the lungs)…. Of course, the customers are not happy!
 Anemia can be caused because someone is not making enough red blood cells, because they are destroying red blood cells before they are actually worn out, because they are making defective hemoglobin or red blood cells, or because they have experienced a great blood loss. Many people are mildly anemic just because they don’t get enough iron in their diet. Remember, iron is needed to make the hemoglobin!
Anemia can be caused because someone is not making enough red blood cells, because they are destroying red blood cells before they are actually worn out, because they are making defective hemoglobin or red blood cells, or because they have experienced a great blood loss. Many people are mildly anemic just because they don’t get enough iron in their diet. Remember, iron is needed to make the hemoglobin!
Platelet – or thrombocytes (throm’-bo-sites) – are the smallest cells in the blood. They are fewer in number than red blood cells, but greater in number than white blood cells. Normally, there are approximately 300,000 platelets in every cubic inch of human blood. Platelets are made in the red marrow of bone and lymph nodes and live for about five to ten days.
Platelets are the “maintenance workers” of the blood. When thrombocytes touch the rough surface of a torn blood vessel, they stick to it and each other. Platelets release factors that form a thread-like substance (fibrin) which forms a clot. The clot hardens into a scab, which covers the breakage until the vessel heals. Then, the clot breaks off and dissolves in the blood. Clotting is very important because without it, blood would continue to flow from the vessel like a leaky hose! Some people are missing some of the factors that produce the clot. They are known as hemophiliacs. When they get cut, they may not be able to stop bleeding.
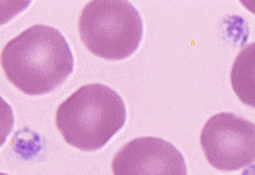 The small purple cells (pictured at left) are platelets. Notice that they are smaller than the red blood cells around them.
The small purple cells (pictured at left) are platelets. Notice that they are smaller than the red blood cells around them.
Medical laboratory scientists may be asked by doctors to count the number of platelets a patient has in their blood. The same instrument that counts the red blood cells can also count platelets. When someone does not have enough platelets, this is known as thrombocytopenia. This can cause a person to bleed excessively after an injury or surgery, because there aren’t enough cells to do the job. There are many different diseases that cause thrombocytopenia.
When someone has too many platelets, this is known as thrombocytosis. It is often a temporary reaction to major trauma (like surgery), and will go away on its own. A small percentage of people with thrombocytosis may make unnecessary clots, which can be very dangerous if they block important blood vessels. If they block heart vessels, they can cause a heart attack.
There are also some inherited diseases that affect platelet quality. Thrombocytopathy is the name for diseases that cause poor platelet quality.
Platelets are very fragile cells and can be greatly affected by drugs. Aspirin, alcohol, and some antibiotics can “hurt” platelets, so they don’t work properly. This means that even though a person may have a normal number of platelets in their blood, they will bleed excessively after an injury because their platelets aren’t doing their job. Even some foods like fish, garlic, and onion, in addition to making your breath stinky, can affect the quality of your platelets if you eat too much of them.
References
- American Society for Clinical Laboratory Science, Clinical Laboratory Science. Flyer. ASCLS Bethesda, MD.
- ASCP Board of Registry, Medical Technologist: A Career for You! Flyer. ASCP Board of Registry, Chicago, IL, 1990.
- Avraham, Regina. The Circulatory System. Chelsea House Publishers, New York, 1989, p. 43-58.
- Diggs, Sturm, Bell. The Morphology of Human Blood Cells, 5th ed. Abbott Laboratories, Abbott Park, IL, 1985.
- Linne, Jean Jorgenson and Ringsrud, Karen Munson. Basic Techniques in Clinical Laboratory Science, 3rd ed. Mosby Year Book, Inc. St. Louis, 1992.
- Lotspeich-Steininger, Cheryl A. et al. Clinical Hematology Principles, Procedures, Correlations. J.B. Lippincott Company, Philadelphia, 1998.
- Purves, William K., et al. Life: The Science of Biology, 4th ed. Sinauer Associates, Inc. Sunderland, Mass., 1995, p. 68-89.
- Sherwood, Lauralee. Human Physiology From Cells to Systems, 2nd ed. West Publishing Company, Minneapolis/St. Paul, 1993.
